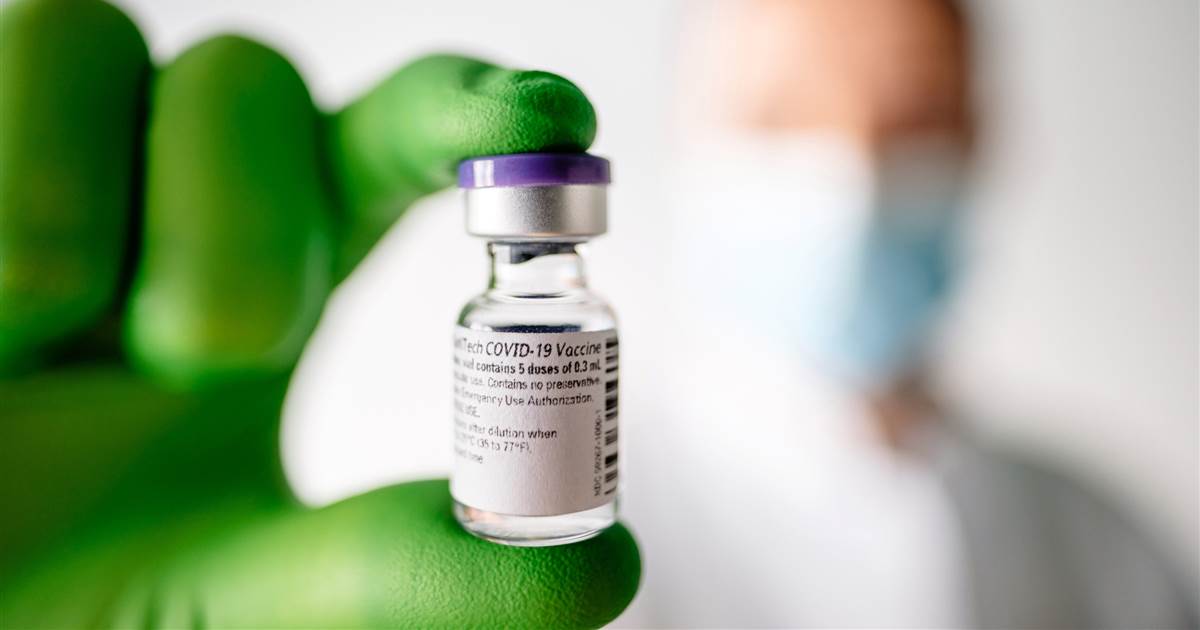
The vaccine rollout crawls forward. Most of us will spend weeks, or months, waiting.
Great Britain did better. As of today, one-third of the English are already vaccinated, twice as many as in America.
Why?
A big reason is that our government decided to rigidly follow its regimen for the Moderna and Pfizer vaccines: two doses, about a month apart.
But why insist on two doses?
The Moderna and Pfizer vaccines are about 90 percent effective after one dose, according to clinical trial data.
British officials sensibly decided to give people one dose, before insisting that everyone get a second dose. It worked. Once people got a first dose, the coronavirus cases began to level off. Although COVID-19 was worse in Great Britain than in America, British cases have now dropped below America’s.
George Mason University economist Alex Tabarrok helped convince British health officials to try the “first-dose-first” approach. But he couldn’t convince American officials.
“We have given out more than 20 million second doses,” Tabarrok complains in my new video. “Those could have been first doses!”
Had they been, 50 percent more Americans would have received a vaccine by now.
“Why would we believe you, rather than these specialist doctors?” I ask.
“Physicians [are] not necessarily thinking about the person who is not their patient,” he replies, “An economist, you’ve gotta be thinking about everybody.”
It’s not too late for America to change policy.
But our government’s planners won’t change without “a proper study.”
In the time the study will take, says Anthony Fauci, “we will already be in the arena of having enough vaccines to go around anyway.”
Tabarrok, wisely, says in a national emergency, we should skip that study and give one dose a real-world test. “You have to act quickly. Bureaucrats are just not used to doing that.”
On TV, Fauci once said: “You can do both! You can get as many people in their first dose at the same time as adhering within reason to the timetable of the second dose.”
But we can’t do both. There are tradeoffs in life.
“We have to take into account scarcity,” says Tabarrok. “This is what economists are good at: thinking about scarcity and thinking about tradeoffs.”
America’s bureaucratic medical approval process is all about following certain rules.
“They’ve been too slow. They’ve made mistakes,” complains Tabarrok. “The FDA did not allow private companies to start testing.”
That meant that for weeks, labs sat idle.
The bureaucracy also slowed the distribution of vaccines.
“We had the doses stockpiled… ready to go. The state governments weren’t ready. They didn’t have websites ready,” Tabarrok points out. “Even though they’d been told months and months, this is coming, vaccines are coming… get ready. And they said, Oh, we don’t have enough money. Give me a break. They have tons of money.”
“They acted more quickly than they usually do,” I point out.
“Not fast enough,” replies Tabarrok.
Fortunately, people outside government stepped up.
Olivia Adams, a software engineer in Massachusetts, got frustrated with her state’s vaccine website and built a site that makes it easier to find COVID-19 vaccine appointments. So did Huge Ma, an engineer in New York.
“It’s been amazing to see how much expertise there is in the world, outside the usual expert channels,” says Tabarrok. “The government has just been behind the virus every single step of the way.”
Fortunately, big greedy corporations were on the ball.
“Thank God for the manufacturers of vaccines for Moderna and Pfizer and Johnson and Johnson that have been the one saving grace in this crisis. Capitalism has brought us the vaccines at a faster pace than ever before. And most of that was due to lifting government regulations.”
He’s right. At the beginning of the pandemic, the FDA lifted regulations, which allowed companies to create vaccines more quickly. Without that freedom, vaccine approval would have taken years.
When the pandemic ends, politicians will take credit, but the solution, as usual, began when politicians got out of the way.